In my last post, we discussed the orientation and philosophy of the personal medical home, as advocated by the American Academy of Family Physicians (AAFP) and the American College of Physicians (ACP). A reasonable question to ask is, what exactly is being done by the doctor and staff that justifies enhanced payment to the physicians office? What are the services that do not fall into the usual payment for an office visit?
Recently, my medical group entered into a pioneering contract with a Medicare Advantage insurance company to hammer out these details as part of a new Medicare Advantage plan. Here is what we came up with:
Personal Medical Home Care Enhancement Services
• Maintain the patient's "personal medical home" electronic health care record, which includes an updated medication list, problem list, and records of all care provided and summaries of care received outside the family physician's office.
• Systematically remind members of covered preventive screening services.
• Apply the Wagner Chronic Care Model of pre-planned office visits to provide medical care for chronic conditions. This model includes the following:
1. A registry system for chronic conditions including but not limited to congestive heart failure and high-risk diabetes, that allows the medical team to identify patients with chronic conditions, assure that the needed care is delivered, and recall the patients for the regular follow-up care necessary for their condition.
2. Software for decision support, available in the room at the time of care. Family Care Network has invested in computerized software that provides evidence-based guidelines for care in the room for patient and health professionals to utilize at the time of services. This software also allows health professionals to link on the web to medical library services from the exam room.
3. The use of clear patient-friendly tools to enable patients to understand their chronic conditions and the actions necessary for them to achieve optimal health.
4. The use of clinical staff to support the patient in self-managing and telephone support, depending on the patient's needs.
• Provide regular quality reports (as agreed) for the insurance companies patients.
• Conduct an annual risk assessment for each member at which time the member's chronic medical problems are identified, reviewed and updated.
• Maintain the patient-doctor health care relationship between office visits by using telephone care and the Doc InTouch secure web messaging system when appropriate. This will enable more frequent interactions with the health care team to facilitate patient self-management.
These "deliverables" for the insurance company are value added work that is in addition to what is normally expected. Taken together, these measures provide a concrete framework that allows for much better patient management, and patient outcomes. If this approach was emulated nationally, it would go a long way to improve our national health care scorecard, and at the same time dramatically improve the financial health of family physician offices.
I believe in a family doctor for every family, lower cost, freedom to choose and coverage for all Americans.
Sunday, December 17, 2006
Tuesday, November 28, 2006
The Medicare Crisis, National in Scope, Local in Impact
Medicare was founded in 1965 to help cover the costs associated with health care for older Americans and those with certain disabilities. Since that time it has evolved into one of the most needed and important programs in U.S. Government history. Unforunately, however, as our nation’s health care system now braces for a Medicare Population explosion, caused by the Baby Boom Generation aging into Medicare, primary care medicine finds itself on the verge of collapse due to drastically insufficient Medicare reimbursement.
Some Medicare beneficiaries have already felt this on a personal level, as they have had difficulty finding a family doctor for their primary care needs. This is due to the fact that Medicare funding for the services provided by family physicians often does not cover the actual cost to the doctor of providing that care! In fact, according to a 2006 report from the American College of Physicians, "Primary care is on the verge of collapse. Very few young physicians are going into primary care and those already in practice are under such stress that they are looking for an exit strategy". The report further notes that the key contributor to the problem they describe is the "inadequate and dysfunctional payment policies" of the government and insurance companies. "Unless immediate and comprehensive reforms are implemented by Congress and CMS (Medicare), primary care - the backbone of the U.S. healthcare system - will collapse," concludes the report. "The consequences will be higher costs and lower quality as patients find themselves in a confusing, fragmented, over-specialized system in which no one physician accepts responsibility for their care, and no one physician is accountable to them for the quality of care provided."
The problem described in this report is very familiar to your family doctor, and all of us here in my practice at Family Care Network (FCN). A Family Medicine practice is really a small business which simply cannot remain viable if revenue does not exceed expense. If the current inadequate and dysfunctional Medicare payment policies continue, and with the Medicare population about to increase dramatically, doctors will have no choice but to close their practice to Medicare patients. It is simply not possible for physicians to subsidize the care of so many without becoming economically non-viable. This is a terrible prospect, at the very time when the need will be the greatest! I believe that this is unacceptable, and that is why I am sharing this information about steps we are taking in my medical group, The Family Care Network Solution.
Family Care Network (FCN) has been working diligently to bring this crisis to the attention of our elected officials. While we sincerely hope that our State and Federal Governments will eventually address this crisis on both a national and local level, we have taken a position that FCN must seek out a more immediate solution to ensure our long term viability for survival.
FCN has developed a long term strategic plan for Medicare which we believe will enable us to:
1. Remain in Practice.
2. Continue practicing family medicine according to the Personal Medical Home model of health care as advocated by the American Academy of Family Physicians (AAFP) (see next page).
3. Continue providing care for our existing Medicare Patients.
4. Care for existing patients who become Medicare eligible.
5. Accept new Medicare patients into our practice (beginning in 2007).
The central component to the FCN Medicare Strategy is partnering ONLY with Medicare insurance companies that recognize the critical role played by family medicine in the overall health care system, and choosing ONLY insurance partners that financially support the "Personal Medical Home" as advocated by the AAFP and ACP.
We realize that patients have different needs and preferences when it comes to their Medicare health insurance. As such, FCN will provide our patients with access to multiple Medicare insurance plan options. We also recognize how confusing Medicare insurance has become and therefore FCN will provide insurance counseling services at no cost to our patients. Licensed insurance professionals well versed in all of the various Medicare insurance plans accepted by FCN, will be on-hand to help you understand your options and enroll in the Medicare insurance plan that is best suited to your personal needs.
Finally, FCN believes that healthy communication correlates directly to healthy patients. FCN requires that all Medicare insurance company partners provide internet connectivity between patient and provider via the DocInTouch web messaging program, at no cost to the patient. DocInTouch is a secure internet-based service that enables patients and physicians to communicate efficiently and effectively, and this type of functionality is part of the personal medical home concept.
All physicians and staff at FCN firmly embrace and support the Personal Medical Home model of health care advocated by the American Academy of Family Physicians (AAFP). FCN supports the Personal Medical Home in the following ways:
1. The physician makes a commitment to the patient to know them as a person, and to provide ongoing, continuity of care for illness and injury, as well as medical planning and advice for screening for illnesses and maintenance of good health.
2. Our office team shares this commitment, assisting the physician in providing hospital care, home care and consultation when needed.
3. Maintain accurate medical records for the care delivered and provide patient education using current technology.
4. Maintain patient registries for certain chronic diseases (Diabetes, Congestive Heart Failure) in order to study, monitor and improve the adequacy of their care, as well as to seek out patients who have not received needed care.
5. Provide planned chronic care visits for diabetes and other appropriate conditions, so that needed information is present for treatment and education at the time of the visit.
6. Integrate patient feedback to improve the performance of the practice.
7. Implement the “New Model of Family Medicine” described in the Future of Family Medicine Report, including secure web messaging.
As we communicate with our patients about these changes, we are letting them know that we greatly appreciate their continued support and patronage. Providing their Personal Medical Home is something that we take very seriously and we remain fully committed to providing the absolute best primary care medicine possible. We recognize that re-evaluating Medicare insurance needs involves significant effort, time and stress. We hope that they understand the challenge we are currently facing, but with stheir support we are confident that we will overcome this challenge, together.
Some Medicare beneficiaries have already felt this on a personal level, as they have had difficulty finding a family doctor for their primary care needs. This is due to the fact that Medicare funding for the services provided by family physicians often does not cover the actual cost to the doctor of providing that care! In fact, according to a 2006 report from the American College of Physicians, "Primary care is on the verge of collapse. Very few young physicians are going into primary care and those already in practice are under such stress that they are looking for an exit strategy". The report further notes that the key contributor to the problem they describe is the "inadequate and dysfunctional payment policies" of the government and insurance companies. "Unless immediate and comprehensive reforms are implemented by Congress and CMS (Medicare), primary care - the backbone of the U.S. healthcare system - will collapse," concludes the report. "The consequences will be higher costs and lower quality as patients find themselves in a confusing, fragmented, over-specialized system in which no one physician accepts responsibility for their care, and no one physician is accountable to them for the quality of care provided."
The problem described in this report is very familiar to your family doctor, and all of us here in my practice at Family Care Network (FCN). A Family Medicine practice is really a small business which simply cannot remain viable if revenue does not exceed expense. If the current inadequate and dysfunctional Medicare payment policies continue, and with the Medicare population about to increase dramatically, doctors will have no choice but to close their practice to Medicare patients. It is simply not possible for physicians to subsidize the care of so many without becoming economically non-viable. This is a terrible prospect, at the very time when the need will be the greatest! I believe that this is unacceptable, and that is why I am sharing this information about steps we are taking in my medical group, The Family Care Network Solution.
Family Care Network (FCN) has been working diligently to bring this crisis to the attention of our elected officials. While we sincerely hope that our State and Federal Governments will eventually address this crisis on both a national and local level, we have taken a position that FCN must seek out a more immediate solution to ensure our long term viability for survival.
FCN has developed a long term strategic plan for Medicare which we believe will enable us to:
1. Remain in Practice.
2. Continue practicing family medicine according to the Personal Medical Home model of health care as advocated by the American Academy of Family Physicians (AAFP) (see next page).
3. Continue providing care for our existing Medicare Patients.
4. Care for existing patients who become Medicare eligible.
5. Accept new Medicare patients into our practice (beginning in 2007).
The central component to the FCN Medicare Strategy is partnering ONLY with Medicare insurance companies that recognize the critical role played by family medicine in the overall health care system, and choosing ONLY insurance partners that financially support the "Personal Medical Home" as advocated by the AAFP and ACP.
We realize that patients have different needs and preferences when it comes to their Medicare health insurance. As such, FCN will provide our patients with access to multiple Medicare insurance plan options. We also recognize how confusing Medicare insurance has become and therefore FCN will provide insurance counseling services at no cost to our patients. Licensed insurance professionals well versed in all of the various Medicare insurance plans accepted by FCN, will be on-hand to help you understand your options and enroll in the Medicare insurance plan that is best suited to your personal needs.
Finally, FCN believes that healthy communication correlates directly to healthy patients. FCN requires that all Medicare insurance company partners provide internet connectivity between patient and provider via the DocInTouch web messaging program, at no cost to the patient. DocInTouch is a secure internet-based service that enables patients and physicians to communicate efficiently and effectively, and this type of functionality is part of the personal medical home concept.
The Personal Medical Home
All physicians and staff at FCN firmly embrace and support the Personal Medical Home model of health care advocated by the American Academy of Family Physicians (AAFP). FCN supports the Personal Medical Home in the following ways:
1. The physician makes a commitment to the patient to know them as a person, and to provide ongoing, continuity of care for illness and injury, as well as medical planning and advice for screening for illnesses and maintenance of good health.
2. Our office team shares this commitment, assisting the physician in providing hospital care, home care and consultation when needed.
3. Maintain accurate medical records for the care delivered and provide patient education using current technology.
4. Maintain patient registries for certain chronic diseases (Diabetes, Congestive Heart Failure) in order to study, monitor and improve the adequacy of their care, as well as to seek out patients who have not received needed care.
5. Provide planned chronic care visits for diabetes and other appropriate conditions, so that needed information is present for treatment and education at the time of the visit.
6. Integrate patient feedback to improve the performance of the practice.
7. Implement the “New Model of Family Medicine” described in the Future of Family Medicine Report, including secure web messaging.
As we communicate with our patients about these changes, we are letting them know that we greatly appreciate their continued support and patronage. Providing their Personal Medical Home is something that we take very seriously and we remain fully committed to providing the absolute best primary care medicine possible. We recognize that re-evaluating Medicare insurance needs involves significant effort, time and stress. We hope that they understand the challenge we are currently facing, but with stheir support we are confident that we will overcome this challenge, together.
Monday, November 27, 2006
How the US Health Care System falls short, and what to do about it!
When most people in the public at large think about our health care situation in the United States, it is usually with regard to the high cost of health insurance premiums. Quality is assumed by most people to be present. Assessment of quality in the US was recently undertaken by the Commonwealth Fund Commission on a High Performance Health System, which has now summarized their results as the National Scorecard on U.S. Health System Performance. This is the first-ever comprehensive assessment of health care outcomes, quality, access, efficiency, and equity in one report. It is no surprise to me that the finding ofthis report show that America's health system falls far short of what we need, especially considering that the US pays more per capita than any other nation on earth.
Across 37 indicators of performance, the U.S. achieves an overall score of 66 out of a possible 100 when comparing actual performance to achievable benchmarks, or a "D+". The following graph shows the score for the US in the major areas observed.
Across 37 indicators of performance, the U.S. achieves an overall score of 66 out of a possible 100 when comparing actual performance to achievable benchmarks, or a "D+". The following graph shows the score for the US in the major areas observed.
Click Graph to Enlarge
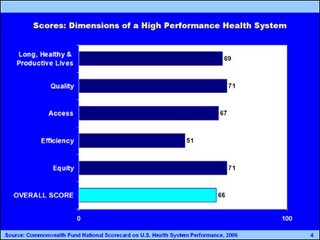 These results clearly show that not only is cost a problem, and not only do we have about 45 million people who are not covered, but our results for the money spent fall far short of what is needed and achieveable.
These results clearly show that not only is cost a problem, and not only do we have about 45 million people who are not covered, but our results for the money spent fall far short of what is needed and achieveable.
I have included a link to the report in this blog, but I believe that the messages from the Scorecard are clear:
Preventive and primary care quality deficiencies undermine outcomes for patients and contribute to inefficiencies that raise the cost of care. These deficiencies are to be expected in a system that chronically underfunds primary care, and does not pay doctors for proven primary care strategies such as electronic medical records, chronic disease registries, telephone management followup, web messaging and quality benchmarks. Universal coverage and participation are essential to improve quality and efficiency, as well as access to needed care.
Quality and efficiency can be improved together, and we must look for improvements that yield both results. Failure to coordinate care for patients over the course of treatment put patients at risk and raise the cost of care. This is especially acute with patients who do not have a "Personal medical home". Policies that facilitate and promote linking providers and information about care will be essential for productivity, safety, and quality gains. Financial incentives posed by the fee-for-service system of payment as currently designed undermine efforts to improve preventive and primary care, manage chronic conditions, and coordinate care. We need to devise payment incentives to reward more effective and efficient care, with a focus on value. Research and investment in data systems are important keys to progress. Investment in, and implementation of, electronic medical records and modern health information technology in physician offices and hospitals is low—leaving physicians and other providers without useful tools to ensure reliable high quality care. By emphasizing adequate payment for primary care, savings can be generated from more efficient use of expensive resources including more effective care in the community to control chronic disease and assure patients timely access to primary care. The challenge is finding ways to re-channel these savings into investments in improved coverage and system capacity to improve performance in the future.
Setting national goals for improvement based on best achieved rates is likely to be an effective method to motivate change and move the overall distribution to higher levels.
Our health system needs to focus on improving health outcomes for people over the course of their lives, as they move from place to place and from one site of care to another. This requires a degree of organization and coordination that we currently lack. It also requires that each person have a "personal medical home" with a primary care physician office team.
This Scorecard is a snap shot of the vital signs of our health system. It is not a pretty picture! Our rising costs and deteriorating coverage require leadership to transform the health system.
I say, let's start by adequately funding all primary care, so that we begin with the basics - adequate access for early care, chronic disease care and preventive care. This personal medical home, supported by state of the art medical records, can then be the organizing central point for improving communication and reforming the health care system.
 These results clearly show that not only is cost a problem, and not only do we have about 45 million people who are not covered, but our results for the money spent fall far short of what is needed and achieveable.
These results clearly show that not only is cost a problem, and not only do we have about 45 million people who are not covered, but our results for the money spent fall far short of what is needed and achieveable.I have included a link to the report in this blog, but I believe that the messages from the Scorecard are clear:
Preventive and primary care quality deficiencies undermine outcomes for patients and contribute to inefficiencies that raise the cost of care. These deficiencies are to be expected in a system that chronically underfunds primary care, and does not pay doctors for proven primary care strategies such as electronic medical records, chronic disease registries, telephone management followup, web messaging and quality benchmarks. Universal coverage and participation are essential to improve quality and efficiency, as well as access to needed care.
Quality and efficiency can be improved together, and we must look for improvements that yield both results. Failure to coordinate care for patients over the course of treatment put patients at risk and raise the cost of care. This is especially acute with patients who do not have a "Personal medical home". Policies that facilitate and promote linking providers and information about care will be essential for productivity, safety, and quality gains. Financial incentives posed by the fee-for-service system of payment as currently designed undermine efforts to improve preventive and primary care, manage chronic conditions, and coordinate care. We need to devise payment incentives to reward more effective and efficient care, with a focus on value. Research and investment in data systems are important keys to progress. Investment in, and implementation of, electronic medical records and modern health information technology in physician offices and hospitals is low—leaving physicians and other providers without useful tools to ensure reliable high quality care. By emphasizing adequate payment for primary care, savings can be generated from more efficient use of expensive resources including more effective care in the community to control chronic disease and assure patients timely access to primary care. The challenge is finding ways to re-channel these savings into investments in improved coverage and system capacity to improve performance in the future.
Setting national goals for improvement based on best achieved rates is likely to be an effective method to motivate change and move the overall distribution to higher levels.
Our health system needs to focus on improving health outcomes for people over the course of their lives, as they move from place to place and from one site of care to another. This requires a degree of organization and coordination that we currently lack. It also requires that each person have a "personal medical home" with a primary care physician office team.
This Scorecard is a snap shot of the vital signs of our health system. It is not a pretty picture! Our rising costs and deteriorating coverage require leadership to transform the health system.
I say, let's start by adequately funding all primary care, so that we begin with the basics - adequate access for early care, chronic disease care and preventive care. This personal medical home, supported by state of the art medical records, can then be the organizing central point for improving communication and reforming the health care system.
Friday, November 24, 2006
How to Lower the Cost AND Improve the Quality of our Health Care

One of my favorite and most useful resources for understanding the complexity and variation in our United States health care "system" is the Dartmouth Atlas of Health Care.
One of the most fascinating observations made as a result of this ongoing study was published in 2004 (Health Affairs, 10.1377/hlthaff.w4.184 Copyright © 2004 by Project HOPE ). The authors, Katherine Baicker and Amitabh Chandra studied the relationship between Medicare Spending, the type of physician workforce, and beneficiary's quality of care. The results were astounding, and showed that only one parameter correlated with improved quality and decreased cost, and that was the ratio of family physicians to the general population.
Click to Enlarge
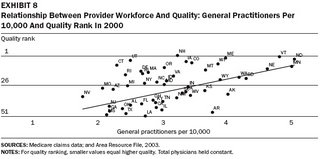
 These results confirm what has also noted all over the world, which is that high functioning health care systems have a high ratio of primary care doctors as part of the physician work force. The authors also looked at the affect of the ratio of more narrowly focused specialist physicians on cost and quality.
These results confirm what has also noted all over the world, which is that high functioning health care systems have a high ratio of primary care doctors as part of the physician work force. The authors also looked at the affect of the ratio of more narrowly focused specialist physicians on cost and quality.Click to Enlarge
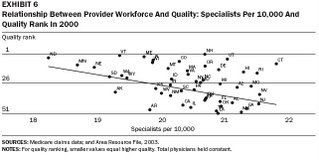
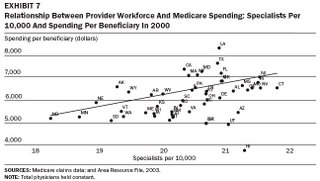 The data clearly show that as the ratio of narrowly focused specialist doctors increases relative to the general population, cost goes up and overall quality actually worsens!
The data clearly show that as the ratio of narrowly focused specialist doctors increases relative to the general population, cost goes up and overall quality actually worsens!How can this be? It seems counter intuitive to many people that more specialists would result in lower quality of care. Based on my years of practice experience, I believe these results are accurate, and that the results are due to several factors:
1.) When family physicians are in short supply, needed primary care services, that should be the foundation of all that we do, are not received by many people who have their first contact with specialists .
2.) When family physicians are in short supply, they are forced into a mode of seeing patients more quickly than is desirable, which I believe lowers the quality and the patient satisfaction. Costs go up because it is easier to simply order the expensive tests that drive up costs than it is to do a detailed history and physical exam before planning workup.
3.) Due to their training and focus, narrowly trained specialists sometimes bring high risk and high expense habits to bear in situations where a less aggressive approach might be preferable.
These doctors are a valuable and needed part of our care delivery system, but they do not specialize in first access health care, screening and helping us to stay well.
The authors looked at other factors, but did not observe any other clear relationships. Data on nurses, for example, did not show a change with a changing ratio to population.
Click to Enlarge
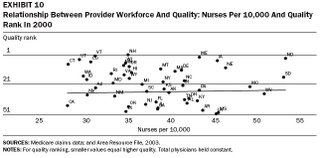 So what does this mean for health care reform? To me, the implications are clear, and aggressive action is required. Health insurers and the federal government need to begin immediately to implement policies that nurture the provision of primary care.
So what does this mean for health care reform? To me, the implications are clear, and aggressive action is required. Health insurers and the federal government need to begin immediately to implement policies that nurture the provision of primary care.Unfortunately, the current state of affairs is bleak. The American College of Physicians (ACP) has issued a 2006 report that predicts the imminent collapse of primary care in the United States, due to the inadequate and dysfunctional payment policies of the government and other third party payers. Most government payment programs do not even cover the overhead cost of doctors to provide primary care, and the situation is getting worse! Medicare, for example, is scheduled to decrease payments by 5.1% as of January, 2007. Fewer and fewer medical students are choosing to pursue family medicine or other primary care as a career option, because they know they can make more money at less personal risk by going into a high tech, limited specialty. Many existing primary care doctors are near retirement and will soon be out of the workforce. And all of this is happening at the very time we will experience a large jump in Medicare age patients needing primary care services.
The Medicare situation is due to the way payments to doctors are calculated. Medicare Part "B" was established to cover doctors visits. As care has become more technical and complex, new services have been added into the pot for coverage. Now, in addition to doctors visits, Par "B" also covers out patient surgery, CT scans, MRI scans, nuclear medicine and other high tech wonders. This then results in Medicare Part "B" spending "too much money", and payment reductions for everyone are then put in place. Primary care office visits get cut back, in spite of the fact that payment is already too low.
If we began a national policy of enhancing the ability of family physicians to provide excellent primary care, it would need to start by decoupling primary care payment from the rest of payment for health care. This would encourage the development of what the American Academy of Family Physicians (AAFP) calls the "personal medical home", a place where they know your name and each of us knows we can go for care and referral. Payment to primary care practices needs to be enough to cover overhead, build state of the art infrastructure to incorporate electronic medical records, support advanced management strategies and let the doctors make a reasonable profit. This will attract doctors to family medicine at the time we need them most! The data are clear. We need to nurture and encourage the only part of our current health care "system" that is already demonstrating a clear relationship to increased quality and lower cost.
Thursday, November 23, 2006
Should Health Care be a Right in the United States?
The United States is very unusual among the industrialized nations of the world, because we are the only country in that group which does not recognize access to health care as a fundamental right of citizenship. How can this be? Why have we evolved in a different direction?
Do you believe that health care should be a right in our country? I do. Some time ago, I submitted an essay to the NPR Radio series, "This I Believe" about my thoughts on this topic. So far, they have not chosen to broadcast my entry, so I include it here.
I was working outdoors in a small courtyard, next to a village school, as a volunteer doctor in El Salvador, when I met an old gentleman who had come to see me. He came accompanied by his daughter, who explained that her father had lost most of his hearing over the last several years, and they had not had the money to have him checked. I finished taking his history, and began my exam, only to find that both of his ears were completely blocked by massive amounts of ear wax. Although the job was difficult, I was finally able to get all of the wax removed, and the joy on his face testified to the miracle he had experienced of being able to hear again. In my lifetime of work as a family physician, I have had many other experiences where the lives of people have been fundamentally changed by receiving needed medical care. I have also seen people whose lives have been changed for the worse when needed care was not available.
I believe that in today’s modern United States, access to medical care must be considered a fundamental right. If the United States of America was founded today, this would be acknowledged in our constitution.
Our founders wrote in the Declaration of Independence:
“ that all men are created equal, that they are endowed by their Creator with certain unalienable Rights, that among these are Life, Liberty and the pursuit of Happiness.”
I believe that 1776 it did not occur to the signers of the Declaration to name medical care as a right, because it barely existed and was not very effective. Rich and poor Americans alike found themselves in the same boat. One in five children died before reaching a year of age, infections and accidents were the leading causes of mortality, and the average age of death was in the early 40s. Indeed, George Washington himself, the founder of our country, died at home from the complications of a strep throat.
Today, our country is much different place. As a family doctor, I have seen first hand how prompt treatment of illness and injury can have life saving and life changing consequences. I have seen how care of chronic illness can prevent disability and premature death, and how screening tests allow us to find and treat early illness to affect a cure. I have witnessed children who became seriously ill due to lack of available treatment or immunizations, and adults who have died from stroke or heart attack because of untreated hypertension. I have seen emergency rooms full of people in crisis with problems that should have been care for in the community long before. In all of these cases, the persons’ ability to exercise their right to “Life, Liberty and the pursuit of Happiness” was taken away by the lack of needed health care.
The Declaration of Independence noted in 1776 that “Governments are instituted among Men” to secure our rights. I believe that health care has now become a basic right, and that it is now time for our government to secure this right for all of us to basic medical care.
This I Believe.

Do you believe that health care should be a right in our country? I do. Some time ago, I submitted an essay to the NPR Radio series, "This I Believe" about my thoughts on this topic. So far, they have not chosen to broadcast my entry, so I include it here.
This I Believe
I was working outdoors in a small courtyard, next to a village school, as a volunteer doctor in El Salvador, when I met an old gentleman who had come to see me. He came accompanied by his daughter, who explained that her father had lost most of his hearing over the last several years, and they had not had the money to have him checked. I finished taking his history, and began my exam, only to find that both of his ears were completely blocked by massive amounts of ear wax. Although the job was difficult, I was finally able to get all of the wax removed, and the joy on his face testified to the miracle he had experienced of being able to hear again. In my lifetime of work as a family physician, I have had many other experiences where the lives of people have been fundamentally changed by receiving needed medical care. I have also seen people whose lives have been changed for the worse when needed care was not available.
I believe that in today’s modern United States, access to medical care must be considered a fundamental right. If the United States of America was founded today, this would be acknowledged in our constitution.
Our founders wrote in the Declaration of Independence:
“ that all men are created equal, that they are endowed by their Creator with certain unalienable Rights, that among these are Life, Liberty and the pursuit of Happiness.”
I believe that 1776 it did not occur to the signers of the Declaration to name medical care as a right, because it barely existed and was not very effective. Rich and poor Americans alike found themselves in the same boat. One in five children died before reaching a year of age, infections and accidents were the leading causes of mortality, and the average age of death was in the early 40s. Indeed, George Washington himself, the founder of our country, died at home from the complications of a strep throat.
Today, our country is much different place. As a family doctor, I have seen first hand how prompt treatment of illness and injury can have life saving and life changing consequences. I have seen how care of chronic illness can prevent disability and premature death, and how screening tests allow us to find and treat early illness to affect a cure. I have witnessed children who became seriously ill due to lack of available treatment or immunizations, and adults who have died from stroke or heart attack because of untreated hypertension. I have seen emergency rooms full of people in crisis with problems that should have been care for in the community long before. In all of these cases, the persons’ ability to exercise their right to “Life, Liberty and the pursuit of Happiness” was taken away by the lack of needed health care.
The Declaration of Independence noted in 1776 that “Governments are instituted among Men” to secure our rights. I believe that health care has now become a basic right, and that it is now time for our government to secure this right for all of us to basic medical care.
This I Believe.

Subscribe to:
Posts (Atom)